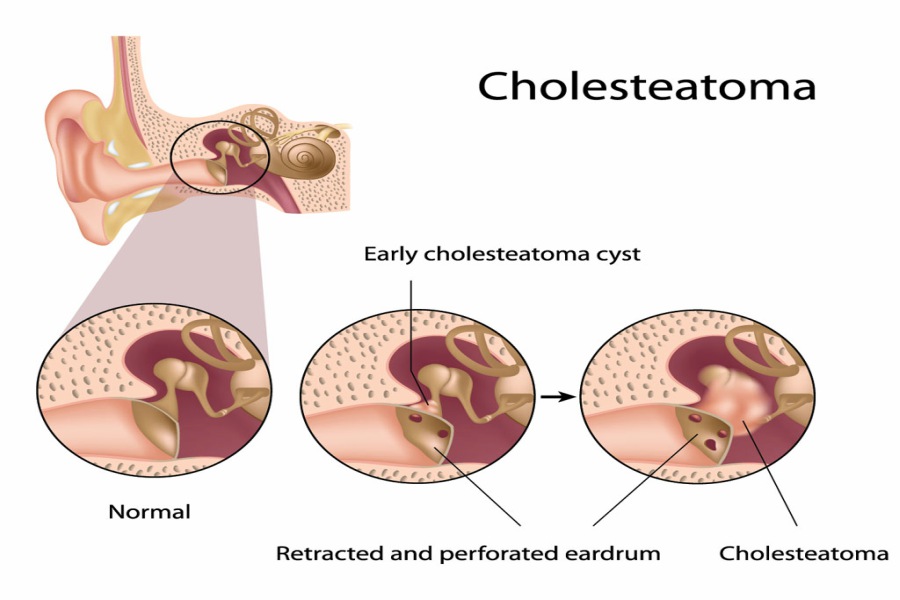
Tympanic membrane (eardrum) is a thin layer of the tissue located deep in the ear canal, which vibrates when the sound waves hit the membrane. The tympanic membrane then transfers the sound waves into the inner ear, which enables us to hear.
Any hole or perforation in the eardrum can affect the hearing ability of a person. The hole in the eardrum can be due to an infection, removal or fall out of ventilation ear tubes, any injury, or growth within or behind the eardrum (cholesteatoma). The hole in the eardrum can cause temporary hearing loss. However, they do not cause complete deafness.
Overview
Tympanoplasty is a surgical procedure performed to repair the defect in the eardrums. It not only closes the hole or perforation but also improves hearing and prevents the water from entering the middle ear. Mostly, a hole in the eardrum of a child gets repaired on its own. If it is not restored even after years, then the eardrum is repaired by a surgical procedure.
ELIGIBILITY
A person can undergo tympanoplasty surgery if he/she has:
- Perforation in the tympanic membrane
- Any lesion involving eardrum or tympanic cavity
- No Eustachian tube dysfunction
But, a person cannot undergo tympanoplasty if he/she has:
- Habit of smoking
- Poor Eustachian functioning
- Undergone multiple attempts for closure previously
- Systemic diseases like diabetes mellitus
- Slag injury
PREPARATION BEFORE PROCEDURE
During your first visit to the doctor, medical history will be obtained. The history and details of the severity of otalgia, hearing loss, vertigo, duration of the perforation or previous attempt at repair will also be obtained. The doctor may also ask about the history of recent infection, and frequency and number of infections. Pneumatic otoscopy and otomicroscopy will be done as a part of physical examination.
Before the surgery, acute or chronic ear infection (if any) will be treated. If the surgery is planned to be done under general anaesthesia, then you will be asked to stop eating before 8 hours of the procedure. Avoid taking any medication that contains aspirin or ibuprofen a week before the surgery.
PROCEDURE TYPE
- Type I tympanoplasty (myringoplasty): In this method, only the perforated area in the eardrum is restored by a graft.
- Type II tympanoplasty: This method is used to treat tympanic membrane perforations along with the erosion of the malleus (ossicle of the middle ear). In this method, a graft is placed onto the remains of the malleus or the incus (bone in the middle ear).
- Type III tympanoplasty: This method is used to treat the defect in which destruction of two ossicles (three bones in the middle ear), but the stapes (bone in the middle ear) still intact and mobile. A graft is placed onto the stapes and protects the assembly.
- Type IV tympanoplasty: This method is used for treating the condition in which ossicular destruction, including part or whole of the stapes arch, has occurred. In this method, a graft is placed around or onto the mobile stapes footplate (present on the right side and head of the stapes).
- Type V tympanoplasty: This method is used to treat the condition in which footplate of the stapes is fixed
ABOUT PROCEDURE
Based on the location and size of the perforation, various techniques and grafting materials can be used.
Based on the type of procedure, it can be done under local or general anaesthesia. The small perforations can be treated by type I tympanoplasty under local anaesthesia along with intravenous sedation. Once the anaesthesia is effective, an incision is made inside the ear canal. The remaining part of the eardrum is raised away from the bony ear canal and elevated forward. With the help of an operating microscope, the surgeon can see the structures of the ear in an enlarged view. For the perforation that is large or at a far distance from the surgeon's view, an incision can be made behind the ear. This aids in providing access to the perforation by elevating the entire outer ear forward. After getting access to the hole, it is rotated forward, and the hearing bones are examined. If any scar tissue is found, it will be removed by laser or the micro hooks. Then the tissue is taken from either a vein or the tragus (a small cartilaginous lobe of skin in the front of the ear) for grafting. To support the graft, an absorbable gelatin sponge is placed under the eardrum. Then the graft is inserted below the remaining eardrum. This remnant of the eardrum is folded back above the perforation to close the hole. Usually, a thin sheet is placed near the top of the graft to prevent its movement.
After completing the procedure, the incision is stitched. In most cases, the stitches are placed in the skin and need not be removed. A sterile patch is placed outside the ear canal.
POST-PROCEDURE CARE
The patient will be transferred to the recovery room after the procedure. Some pain killers and antibiotics will be prescribed to reduce pain and infection. Mostly, it is an outpatient procedure, and the patient will be allowed to go home after a few hours. The patient will be called for a follow-up visit after ten days in which the packing outside the ear will be removed. After removing the packing, the ear will be examined to see if the graft is successful. After three weeks, under the operating microscope, complete packing will be removed.
RECOVERY TIPS
Following measures may aid in speedy recovery after tympanoplasty:
- Prevent the ear from any kind of infection
- Keep the ear dry for at least a few months
- Prevent the ear from excessive tension and shearing forces
- Avoid doing activities that may change the tympanic pressure
- Go for follow-up visits as scheduled by the doctor
FACTORS AFFECTING COST
The cost of tympanoplasty may vary depending on the several factors like:
- Severity of the condition
- Type of the procedure
- Size of the eardrum perforation
- Location of the perforation
- Type of the hospital
- Surgeon
- Hospital stays (if required)
FAQ
Tympanoplasty may be associated with the complications, such as:
- Failure of the graft to heal
- Narrowing of the ear canal
- Recurrent eardrum perforation
- Scarring or adhesions in the middle ear
- Hearing loss
- Perilymph fistula
- Extrusion or erosion of the prosthesis
- Displacement of the prosthesis
- Facial nerve injury
Activities like the use of straw for drinking, sneezing with mouth shut, or heavy nose blowing can change the tympanic pressure. Therefore, these activities should be avoided after tympanoplasty.
In most of the cases, it takes around 2 to 3 hours to complete.
Yes, he can go swimming, but only when his doctor permits.
No, not all eardrum perforations lead to hearing loss. It basically depends on the location and size of the perforation.


 Best Hospitals
Best Hospitals












