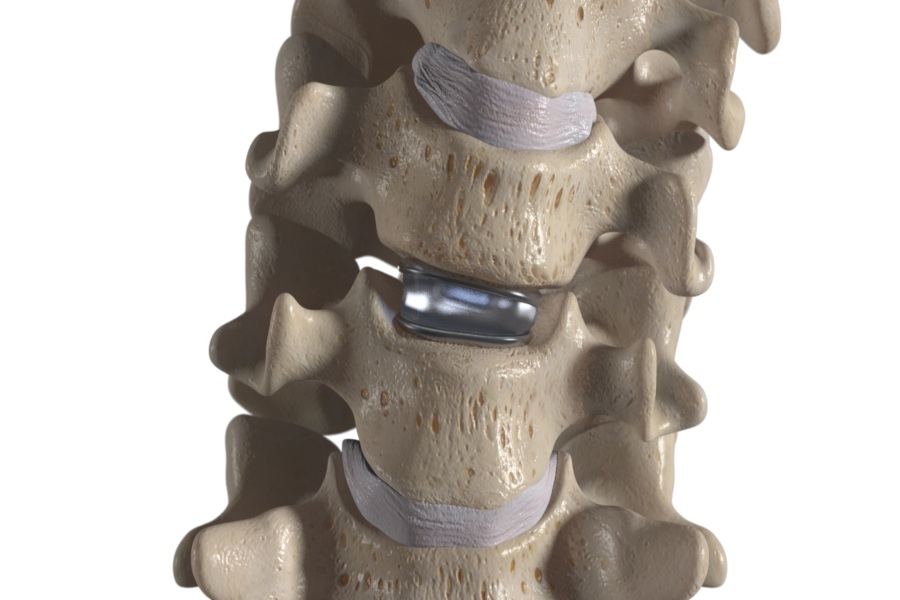
Overview
A human spine is made up of several bones called vertebrae, which are arranged on top of each other. The cervical spine is made up of 7 vertebrae, which form the neck area, and the lumbar spine consists of 5 vertebrae, which form the lower back.
Between these vertebrae, there are discs that act as cushions, allowing the vertebrae to move and rotate without rubbing against each other. The disc has an inner gel like portion and an outer hard and strong portion.
Over the years, the discs degenerate. The outer hard cover starts to weaken and develop cracks. This allows the inner soft material to bulge out of the cracks and eventually cause compression of the spinal nerves and spinal cord. This causes pain, weakness or numbness in the back. When the nonsurgical treatments fail to reduce the symptoms, disc replacement surgery is recommended.
Disc replacement surgery involves replacing a degenerated disc with an artificial disc made up of metal or plastic and metal combination.
Traditionally, when a damaged disc causes severe pain, the disc is removed, and the adjacent vertebra are fused; this reduces pain but at the same time limits the movement of the spine. Disc replacement helps to reduce pain and to restore motion of the spine
ELIGIBILITY
Individuals with the following criteria are eligible to undergo a cervical disc replacement surgery:
- One or two cervical spine discs are degenerating that are compressing nerve roots and herniating, causing arm pain.
- Conservative treatments like pain medication physical therapy, or neck bracing have shown no improvement.
- Overall good health with no indications of osteoporosis, arthritis, infection, or osteomalacia.
One is considered a good candidate for lumbar disc replacement if:
- Degeneration of one or two discs in the lower spine is causing back pain.
- No significant nerve compression
- Not diagnosed with scoliosis, any spinal deformity or other spinal diseases
PREPARATION BEFORE PROCEDURE
After initial physical examination and review of medical history, tests like X-rays, CT or MRI scan, or discography may be recommended. These tests allow the doctor to view the spine and understand the nature and extent of the spinal damage, source of the pain, thereby helping to plan the surgery.
Before the surgery, your doctor might give specific instructions to prepare you for the surgery.
Some of the common steps to prepare for the surgery include:
- Inform your doctor if you are taking any medications, including aspirin, over-the-counter medications, vitamin supplements, or herbal supplements. Some of these medicines may affect the blood clotting and healing process, so you may be asked to stop taking them prior to surgery.
- Tell your surgeon if you or anyone from the family has a history of reaction to general anaesthesia.
- You may be asked to stop smoking before and sometime after the surgery.
- You may be asked not to eat or drink anything for a few hours before the surgery. Usually, it is recommended not to eat or drink after midnight on the night before surgery.
- Ask your doctor what medications you can take on the day of the surgery.
ABOUT PROCEDURE
Although the site of surgery of cervical and lumbar disc replacement vary, the basic technique of the surgery remains the same.
The following are the fundamental steps of a disc replacement surgery:
- An intravenous (IV) vein is put in the hand or arm, through which the anaesthesia and other medicines are given.
- An incision is made on the front or side of the neck (for cervical) or in the abdomen (for lumbar), depending on the location of the damaged disc.
- The important organs and blood vessels are carefully moved to the side to access the spine.
- The damaged disc will be removed, and the artificial disc is secured in the position.
- The organs and blood vessels are put back in place, and the incision is closed with absorbable sutures or stitches.
- The surgical site will be wrapped with a dressing, and you will be moved to the recovery room.
POST-PROCEDURE CARE
After the surgery, you will be moved to the recovery room, where you will be closely monitored. You will wake up after the effects of anaesthesia wear-off. You may have the IV line and a urine catheter in place. You might have to stay in the hospital for a day or two.
Pain medicines will be given if needed. You will be encouraged to get out of the bed and walk within the first day of the recovery period. Your IV line and catheter may be removed in a few days of surgery. If you have undergone cervical disc replacement, a support collar might be given.
You will be shown some exercises and to help you recover faster. As you recover, you will be encouraged to walk and stretch. You will be asked to avoid any sudden or jarring movements for a while. After a few weeks, you can start physical therapy.
Talk to your surgeon about the activities you should avoid and when you can take a shower or bath.
RECOVERY TIPS
Your doctor may give you some specific guidelines to speed up your recovery. Here are some general instructions:
- Ensure that you rest well before taking part in any physical exercise
- Take the prescribed medications regularly
- Clean the surgical site every day, as per the instructions given by the doctor
- Consume foods rich in essential vitamins and minerals, eat more of fruits and vegetables, and stay hydrated
- Attend all the physical therapy sessions and follow the instructions given by your therapist to perform the exercises correctly at home
FACTORS AFFECTING COST
The cost of disc replacement surgery depends upon:
- The location of the hospital
- The type of surgery
- Type of anaesthesia used
- The surgeon
FAQ
Usually, artificial disk replacement surgeries require 2 to 3 hours. However, the duration may vary based on the patient’s condition and the type of surgery performed.
Some of the possible complications of cervical disc replacement include:
- Reactions to the anaesthesia
- Allergic reaction to the materials of the disc
- Infection of the surgical site
- Bleeding
- Spinal fluid leakage
- Nerve injury
- Voice change
- Stroke
- Loosening or breaking of the artificial disc
- Failure to relieve symptoms
- Tingling or numbness in the extremities
- Paralysis
Some of the potential risks of lumbar disc replacement include:
- Infection of the artificial disc
- Dislocation of the artificial disc
- Failure or fracture of the implant
- Allergic reaction to the materials of the disc
- Loosening of the implant
- Breakdown of the spinal bones causing narrowing of the spine (stenosis)
- Problems caused by a poorly placed implant
- Rigidity or stiffness of the spine
- Blood clots in the legs because of decreased activity
- Sexual dysfunction in males
- Nerve damage
- Slow intestinal movement
The duration of recovery is different for various patients based on their age, overall health and their lifestyle; it may vary from a few weeks to a few months. However, one should be able to return to the normal activities within 4 to 6 weeks.
Call your doctor immediately if you have:
- Redness, swelling, bleeding, or discharge from the incision site
- Severe pain that does not respond to the prescribed pain relievers
- Fever or headache
- Weakness or numbness
- Hoarseness
- Difficulty in breathing or swallowing


 Best Hospitals
Best Hospitals













